Vaccination against the human papillomavirus (HPV) remains one of the most widely discussed topics in modern medicine. At the centre of this debate is Gardasil − a vaccine that has drawn a broad range of opinions, from unequivocal support to notable scepticism. An objective assessment requires reliance on verified medical evidence and international health guidelines.
Gardasil is a prophylactic vaccine designed to prevent infection by the most dangerous strains of HPV. The current formulation − Gardasil 9 − offers protection against nine HPV types, including types 16 and 18, which research indicates are responsible for approximately 70% of cervical cancer cases, as well as types 31, 33, 45, 52, and 58, which are associated with additional oncological risks. The human papillomavirus is also linked to cancers of the anal canal, oropharynx, and male genitalia, as well as the development of genital warts. It is essential to emphasise that the vaccine has no therapeutic effect and does not act on an existing infection − it serves exclusively as a preventive measure.
The vaccine's efficacy is greatest when administered before any possible exposure to the virus, which explains the recommendations for early vaccination. International health organisations indicate that the optimal age for vaccination is between 9 and 12 years, when the body's immune response is most robust. Vaccination is also widely recommended up to age 26, while for older individuals its appropriateness is determined on a case-by-case basis, as the likelihood of prior viral exposure increases. The minimum approved age is nine years, and use of the vaccine beyond age 45 remains insufficiently studied.
Vaccine safety is one of the central questions in public discourse. Gardasil has been in global use for more than 15 years, during which hundreds of millions of doses have been administered. The vaccine contains no live virus and cannot cause infection. Accumulated data from clinical trials and post-marketing surveillance demonstrate a favourable safety profile. The most common adverse reactions are mild and transient, including pain at the injection site, fatigue, and a slight increase in body temperature. Serious complications, such as severe allergic reactions, are extremely rare.
There are also clearly defined contraindications. Absolute contraindications include severe allergic reactions to vaccine components or anaphylaxis following a previous dose. Acute infectious illness, elevated temperature, or exacerbation of chronic conditions may serve as temporary grounds for postponing vaccination. As a general rule, vaccination is deferred during pregnancy. In every individual case, the decision should be made by a physician taking all relevant factors into account.
The risks associated with declining vaccination merit particular attention. HPV is one of the most prevalent sexually transmitted infections, and the likelihood of lifetime exposure to the virus remains high. Forgoing prevention means retaining the risk of precancerous changes and virus-associated malignancies. Vaccination, on the other hand, can substantially reduce these risks, particularly when administered within the recommended timeframe.
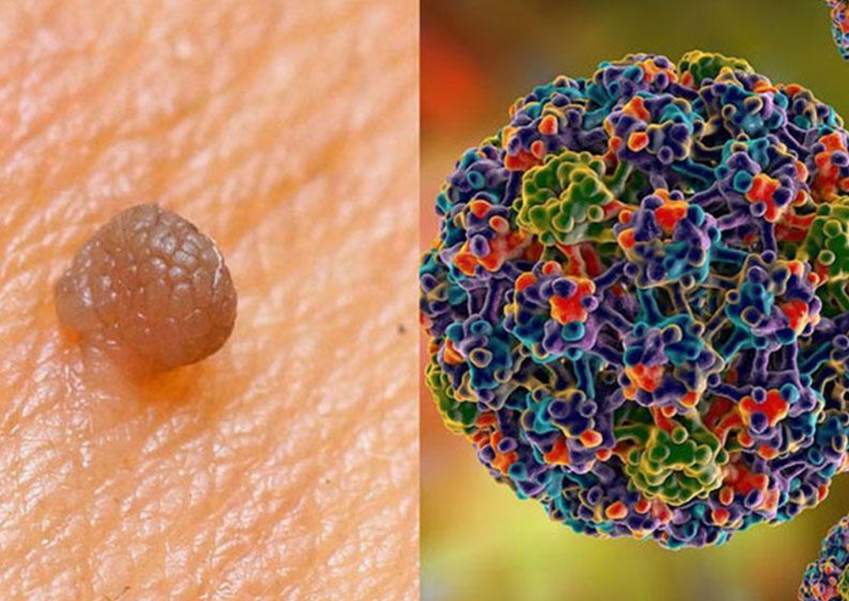
It is important to note that vaccination does not eliminate the need for regular screening. Since the vaccine does not protect against all oncogenic HPV types, women are still advised to undergo routine cytological examinations (Pap smears) and other forms of cervical cancer screening in accordance with established medical protocols.
Despite a substantial body of evidence, myths continue to circulate around the vaccine, including claims linking it to infertility or serious long-term consequences. To date, no such claims have been substantiated by scientific data. The position of the international medical community remains unequivocal: the HPV vaccine is regarded as an effective preventive measure.
In summary, Gardasil represents a scientifically grounded tool for reducing the risk of several oncological diseases. However, as with any medical procedure, the decision to vaccinate should be made on an individual basis, following consultation with a qualified specialist and with full consideration of all relevant indications and contraindications.




















